A glance at Vitamin D and goitrogenic meals in thyroid condition!
This blog post may contain affiliate links. If we find a product or service to be useful, we encourage you to visit the website via that link. If you make a purchase through our referral link, we may receive a commission. Rest assured, you will not be charged any additional fees. By using these links, you can support us while making your purchase. For more information visit here.
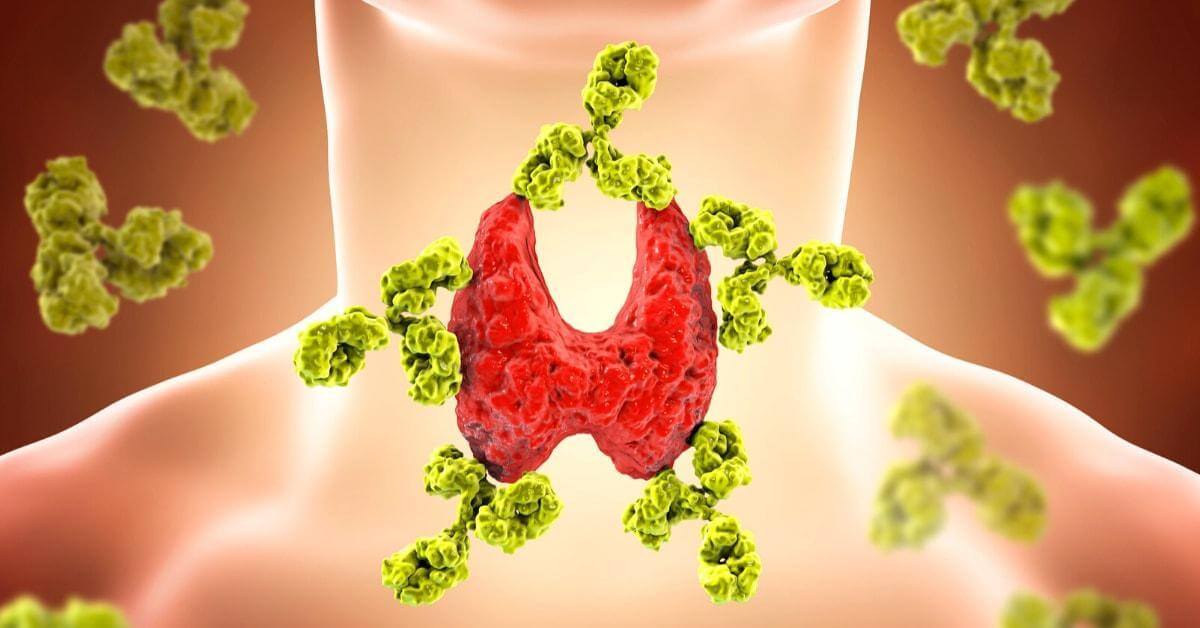
How Goitrogenic Meals Affect Thyroid Health
Let’s have a look at Vitamin D and goitrogenic meals for thyroid conditions! Goitrogens are naturally occurring compounds in some plants. Animal studies suggest these foods may interfere with the absorption of iodine, which is essential for the thyroid to function well.
Goitrogens disrupt the composition of thyroid hormones by interfering with the iodine uptake by the thyroid gland. That triggers the pituitary gland to release thyroid-stimulating hormone (TSH), which then promotes the germination of thyroid tissue, eventually leading to goiter.
Without adequate iodine, the pituitary gland produces thyroid-stimulating hormone (TSH), which promotes the growth of thyroid tissue and eventually leads to gland enlargement, or goiter. If the goiter becomes large enough, it can obstruct the trachea and gastrointestinal tract, causing coughing, trouble eating, and breathing.
Despite this, any substance that interferes with thyroid function is a concern for patients with thyroid autoimmune diseases such as Hashimoto’s thyroiditis and Graves’ disorder. Some people already have thyroid hormone production issues.
Which Plants Are Goitrogenic?

Several animal studies suggest that the following raw cruciferous vegetables affect iodine intake and thyroid metabolism:
Bamboo shoots, Bok Choy, brassica seeds, Broccoli, Brussel sprouts, Cabbage, Cassava, Cauliflower, kohlrabi, Mustard and mustard greens, Peach, Radish, Rutabagas, Soy and soybean products, Spinach, Strawberries, turnip, and many more, are known to have Goitrogenic properties.
What does this mean for thyroid patients?
You’ve probably read this list and thought, “Why can’t I eat these foods when they’re supposed to be healthy for me?” and appropriately so. After all, many of these foods are rich in vital nutrients essential for your health. Limited research so far does not suggest that eating these foods in moderation inhibits thyroid activity.
Yet, a diet that relies heavily on goitrogenic foods can negatively affect patients with autoimmune thyroid disorders. A tailored diet for optimal thyroid function makes more sense than a comprehensive elimination of these foods. A single human study has not confirmed that cruciferous vegetables can decrease thyroid function in humans.
Fifty years of research by Dr. Joel Fuhrman show that these are not “harmful” foods. They may not be the right food for special people. He says that “cruciferous vegetables can be detrimental to thyroid function only in cases of iodine deficiency or insufficient iodine intake” and may not cause any problems if consumed in appropriate amounts.
How much can I eat?
Unfortunately, there is no simple answer to this question, as each patient is different. However, finding what works best for you is possible within the functional model of care. Most patients with thyroid conditions can tolerate raw goitrogenic foods once or twice daily with no problems. Others may need to heat their green vegetables to overcome their goitrogenic activity. Fermented soy is preferable if a patient wishes to include soy in their diet.
Yet, some evidence suggests that soy and soybean products may interfere with the absorption of thyroid medication in hypothyroid patients. Patients should not rely too much on soy in their diet as it is goitrogenic. Eating a few servings of these foods shouldn’t be a problem, whether you have Hashimoto’s thyroiditis or Graves’ disease.
However, they affect iodine metabolism and increase the risk if you already have an iodine deficiency. Even though cooking these foods can reduce goitrogenic activity, avoid eating too many of these foods. Discuss your concerns with your practitioner or doctor and work with them to create a diet chart that works best for you.

Significance of Vitamin D in Thyroid Conditions
You know that vitamin D is responsible for managing calcium in the abdomen, bones, skin, blood, and disease resistance. Yet, several studies suggest that vitamin D levels may contribute to many other health problems.
Researchers now believe that it plays a vital role in communication between cells. Clinical studies link abnormal vitamin D levels to colon, prostate, breast cancers, heart disease, weight gain, and thyroid conditions.
Vitamin D production
Vitamin D is uncommon compared to other vitamins because it is nearly impossible to get what you need from food. Instead, when exposed to natural or artificial UVB light, your body produces it naturally through the skin. Once your body absorbs vitamin D or accepts it as a supplement, it is transmitted to the liver. The liver converts vitamin D to 25(OH)D, sends it to different body areas, and activates it. Once activated, it starts working immediately.
Auto-Immune Conditions
Autoimmunity occurs when the immune system perceives a person’s healthy tissues and cells as threats. When this happens, their body creates an immune response and attacks. This reaction can cause damage, inflammation, and chronic pain in many parts of the body. Vitamin D deficiency can reduce the body’s ability to fight infections such as Hashimoto’s thyroiditis and Graves’ disease.
Clinical studies
The researchers measured several factors associated with the thyroid, including vitamin D3. Vitamin D is a group of compounds classified as vitamins D1, D2, and D3. Vitamin D3 is the naturally occurring form of the vitamin and is the most biologically active. Researchers found that patients with autoimmune thyroid disease had significantly lower levels of vitamin D3 than healthy controls.
Patients with high thyroid peroxidase antibodies the body produces in autoimmune thyroid disease also have low levels of vitamin D. This suggests that vitamin D deficiency may be associated with or cause autoimmune thyroid disease.
Brazilian researchers examined 54 Hashimoto’s patients compared to 54 healthy controls. They found vitamin D deficiency in 63.2% of patients. Those with low vitamin D levels also had higher levels of thyroid-stimulating hormone and an enlarged thyroid.

Vitamin D deficiency
Usually, the skin produces enough vitamin D when exposed to enough UV light. Yet, skin cancer or melanoma risk now means that many people use sunscreen and cover their bodies. However, we also spend more time inside our homes for work and entertainment.
As more clinical trials show a link between vitamin D and thyroid function, many physicians now recommend vitamin D testing as part of thyroid evaluation and care. Still, functional therapists and doctors who follow the medical model may treat you differently based on your results.
Medical Model vs Functional Model
The medical model recommends 400 international units of vitamin D per day. They define an excellent serum 25(OH)D level as more significant than 50 nmol/L because it “meets the needs of 97.5% of the population”. The 25-hydroxy vitamin D blood test is used to measure vitamin D levels.
The medical paradigm frequently recommends supplementation to increase low vitamin D levels. Yet, the functional approach to care recognizes several causes that can lead to low vitamin D levels. As a result, recommending supplements can be ineffective and counterproductive before overall health and other potential issues are seen.
Supplements do not permanently cure low vitamin D levels because they do not address the underlying problems. Some autoimmune patients may not activate the vitamin D receptor because of variations in their DNA sequence.
Also Read: Can You Treat Thyroid With Ayurveda, The Main Causes & Symptoms?
As a result, they require higher than normal vitamin D blood levels to avoid vitamin D deficiency. Vitamin D is fat-soluble, and some patients with thyroid issues, such as Hashimoto’s thyroiditis, have less stomach acid and decreased fat absorption.
Autoimmune conditions such as Hashimoto’s thyroiditis and Grave’s disease also cause the immune system to work overtime. This depletes the body’s vitamin D. Therefore, addressing gut and digestive issues and modulating the immune system is primary before considering vitamin D supplementation.

A highly qualified functional doctor will look at your gut and digestive health, and if not satisfied, they may order a 25-hydroxy vitamin D blood test for your vitamin D levels.
How do goitrogenic meals and Vitamin D affect the thyroid condition?
As needed by the body, your doctor may recommend supplementation between 60 and 80 nmol/l. It is still well below the 125 nmol/L threshold where a patient may experience adverse effects. After several months, they will retake the test. If their serum level rises to an acceptable level, the doctor will adjust their vitamin D intake, so the serum level remains between 50 and 60 nmol/L.
Vitamin D deficiency is just one factor contributing to thyroid problems, so we do not recommend it as a self-supplementation because it may be ineffective if the underlying problems persist. Discuss your thyroid issues with a functional doctor to develop an effective treatment protocol. This is how goitrogenic meals and Vitamin D affect thyroid health.
Did it help you? If you liked this, let us know. Thank you for reading this article. You can send us your suggestions or experiences as comments, and we will feel exceptional.
Understanding the importance of copyright law is absolutely vital, as it strictly prohibits any reproduction or replication of works without the explicit permission of the author. Any unauthorized duplication of content will lead to legal action for copyright infringement under Section 14 of the Copyright Act.